Perimenopause Is an Inflammatory Event: What the Research Says (and What You Can Do About It)
A Registered Dietitian’s Evidence-Based Guide to the Inflammatory Shift Behind Your Symptoms
If you’re somewhere in your forties and your body suddenly feels like a stranger — joints that ache for no reason, brain fog that makes you question your own competence, sleep that abandoned you without warning, mood swings that don’t match your life, fatigue that laughs at your third cup of coffee, and maybe hot flashes layered on top of all of it — you’ve probably been told these are separate problems.
Maybe you’ve gotten separate advice for each one. Melatonin for sleep. An antidepressant for mood. Ibuprofen for joints. “Try to relax” for the hot flashes. And when you asked why everything seemed to change at once, you got some version of “well, you’re getting older” or “this is just perimenopause.”
Here’s what I want you to know: these symptoms aren’t separate. They’re connected. And the connection isn’t vague or hand-wavy. It’s a specific, measurable, well-documented biological process.
That process is inflammation.
Short on Time? Do These Three Things First.
- Add ground flaxseed (2 tablespoons daily) to your morning oatmeal, yogurt, or smoothie. It’s one of the most anti-inflammatory foods for this transition. (Full guide here.)
- Build anti-inflammatory plates — half vegetables, quarter protein, quarter whole grains, plus a healthy fat like
olive oil or avocado. Do this at lunch and dinner this week.- Walk for 20 minutes today. Regular movement measurably reduces the inflammatory markers driving your symptoms. Consistency beats intensity.
Start with these. Then come back when you’re ready.
This post may contain affiliate links to products that align with my evidence-based nutrition approach. As an Amazon Associate I earn from qualifying purchases. Full disclosure.
The Part Nobody Explains at Your Doctor’s Appointment
Most conversations about perimenopause focus on hormones — estrogen going down, periods getting unpredictable, and the reproductive changes that come with that. That part is accurate, but it’s only half the story.
Here’s the other half: estrogen isn’t just a reproductive hormone. It’s one of your body’s most powerful anti-inflammatory regulators.
Think of estrogen as the chief of your body’s fire department. For decades, it’s been patrolling your systems — your brain, your joints, your gut, your heart, your bones — keeping small inflammatory fires under control before they spread. When estrogen starts to fluctuate and decline during perimenopause, that fire chief goes part-time. Then eventually retires.
And the fires start to smolder.
A landmark 2020 review in the Journal of Neuroinflammation put a name to this: the researchers described perimenopause as a “systemic inflammatory phase.” They documented how falling estrogen activates something called the inflammasome — your body’s most sensitive alarm system for threats — which then ramps up production of inflammatory chemicals called cytokines, including IL-6 and TNF-α (McCarthy & Raval, 2020).
Then in 2025, the SWAN study — one of the longest-running studies of women’s health through menopause, tracking over 3,000 women across 21 years — confirmed it with hard data. They found that inflammatory markers like C-reactive protein (CRP) and IL-6 show significant increases around the final menstrual period. And here’s the part that really matters: some women showed rising inflammation years before menopause was technically “official” (El Khoudary et al., 2025).
So if you’ve been feeling like something is off but your labs look “normal” and you’re told you’re not in menopause yet — your inflammation may already be rising. You’re not imagining it. The science backs you up.
One Fire, Seven Floors: How Inflammation Creates All Your Symptoms
Here’s the analogy that helps my clients understand this: imagine a building with a slow fire burning in the basement. The fire is in one place — but smoke reaches every floor. On one floor, the smoke detector goes off (hot flashes). On another, the air quality drops (brain fog). On another, the paint starts peeling (joint pain). On another, the lights flicker (mood changes).
If you only deal with each floor’s problem individually — a new smoke detector here, an air purifier there — you never address the fire. But if you address the fire itself, every floor gets better.
That’s inflammation during perimenopause. Let me walk through each “floor.”
Hot Flashes and Night Sweats
Your brain has a thermostat (the hypothalamus) with an acceptable temperature range. When estrogen declines and inflammation rises, that range shrinks dramatically — like going from a comfortable 68-72°F window to a ridiculously narrow 70-70.5°F. The slightest temperature fluctuation triggers an emergency cooling response: blood vessels dilate, sweat glands activate, and you get a hot flash.
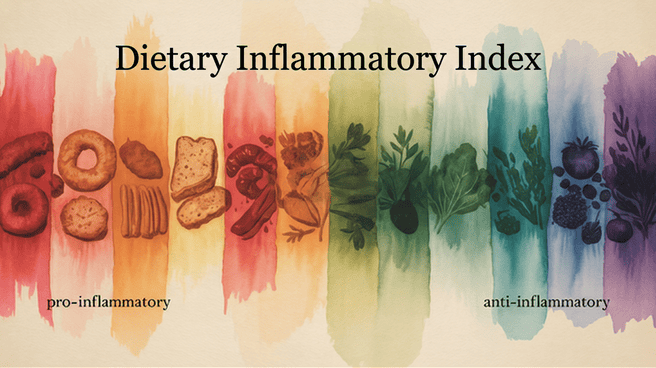
The inflammation connection isn’t theoretical. A 2023 study found that women with more pro-inflammatory diets — measured using the Dietary Inflammatory Index — had significantly worse hot flashes and night sweats (Haghshenas et al., 2023). And the WAVS trial showed that an anti-inflammatory, plant-based diet with daily soybeans reduced moderate-to-severe hot flashes by 88% over twelve weeks (Barnard et al., 2023).
That’s not a subtle effect. That’s food changing the inflammatory environment enough to dramatically reduce symptoms. (I’ve written a complete deep dive on this research if you want the full breakdown.)
Joint Pain and Stiffness
This is one of the most under-recognized perimenopausal symptoms. Many women in their forties develop new joint pain — hands, knees, shoulders — and assume it’s arthritis or just aging. But the timing often aligns precisely with the hormonal transition, and the mechanism is inflammatory.
Estrogen directly protects your joints. It maintains cartilage, supports the production of synovial fluid (the natural lubricant inside your joints), and dampens inflammation in the tissue lining your joint capsules. When estrogen declines, you lose that protection — and the inflammatory cytokines that are now running higher go straight for your joints.
This is worth knowing because it means the same anti-inflammatory approach that helps with hot flashes may also help your joints feel better. Same fire, different floor.
If your joint pain is new, persistent, or severe — please get it evaluated. It’s important to rule out specific conditions like rheumatoid arthritis. But it’s also important to know that perimenopausal joint inflammation is real and treatable.
Brain Fog and Cognitive Changes
This is the one that scares women the most. Walking into a room and forgetting why. Losing words mid-sentence. Reading the same paragraph three times. The fear — “Is this early dementia?” — is almost always unfounded. But the symptom is real, and it has a biological basis.
Estrogen supports your brain in ways that go far beyond reproduction. It promotes the neurotransmitters that keep your thinking sharp (serotonin, norepinephrine), protects the blood-brain barrier, and supports the connections between your brain cells.
When estrogen drops, those systems weaken. But here’s the less commonly discussed factor: inflammatory chemicals can cross the blood-brain barrier and directly inflame brain tissue. This affects the hippocampus — the region responsible for memory and recall — which is exactly why you’re forgetting things (McCarthy & Raval, 2020).
The fact that you’re reading this and learning about neuroinflammation puts you way ahead. Most women are told “it’s just stress” and sent on their way. You now understand the mechanism — which means you can address it.
Omega-3 fatty acids (particularly DHA) are major structural components of brain cell membranes. Mediterranean-style eating patterns — which are fundamentally anti-inflammatory — have been consistently linked to better cognitive outcomes. These aren’t coincidences.
Mood Changes, Anxiety, and Low Mood
Here’s something that changes how you think about perimenopausal mood changes: inflammation literally steals the raw materials your brain needs to make serotonin.
Under inflammatory conditions, an amino acid called tryptophan — the building block of serotonin — gets diverted away from serotonin production and into something called the kynurenine pathway. This pathway produces inflammatory compounds instead of the neurotransmitter that keeps your mood stable. More inflammation = less tryptophan becomes serotonin = lower, more unstable mood.
Add in the direct effects of fluctuating estrogen on serotonin receptors and norepinephrine production, and the mood changes of perimenopause make complete biological sense. These aren’t character flaws. They’re predictable biochemistry.
Meta-analyses have found that omega-3 supplementation — particularly EPA — has a modest but meaningful benefit for depression. This makes sense: EPA is anti-inflammatory, and inflammation is disrupting serotonin production through that tryptophan-stealing pathway.
An important note: Anti-inflammatory nutrition can support mood during perimenopause, but it’s not a substitute for mental health care. If you’re experiencing significant depression, persistent anxiety, or emotional changes that affect your daily life, please talk to a mental health professional. Therapy, medication when indicated, and nutritional support work together — not as alternatives to each other.
Sleep Disruption
Sleep and perimenopause have a particularly vicious relationship — and inflammation is the thread running through it.
Night sweats fragment your sleep. Fragmented sleep raises cortisol. Higher cortisol promotes inflammation. More inflammation worsens night sweats. The cycle feeds itself.
But it’s not just night sweats. Inflammatory chemicals themselves disrupt melatonin production and circadian signaling — the internal clock that tells your body when to sleep and when to wake. And cortisol, which rises with both stress and inflammation, directly opposes melatonin. When cortisol is elevated at night, melatonin can’t do its job.
This is why improving sleep during perimenopause usually requires more than one strategy: temperature management (cool bedroom, moisture-wicking sheets), timing your last meal (avoid eating close to bedtime), magnesium glycinate supplementation (which supports both sleep quality and inflammation reduction), and tart cherry juice as one of the few natural dietary sources of melatonin. (I have a detailed look at tart cherry juice for sleep and hot flashes if you’re curious about the evidence.)
If your sleep disruption is severe, persistent, or accompanied by snoring or excessive daytime sleepiness, please get evaluated for sleep apnea — it becomes more common during and after the menopausal transition.
Weight and Body Composition Changes
If your body has shifted during perimenopause — particularly around the midsection, despite no changes in diet or activity — inflammation is part of the mechanism. And I want to name this clearly: what’s happening to your body is not your fault.
Here’s the biology: systemic inflammation promotes insulin resistance. When your cells become less responsive to insulin, your body produces more of it. Chronically elevated insulin drives fat storage, especially visceral fat — the metabolically active fat around your organs and midsection. Simultaneously, elevated cortisol (from inflammation, poor sleep, and the cumulative stress of feeling unwell) also drives visceral fat accumulation.
This double mechanism explains why perimenopausal body changes feel qualitatively different from anything you’ve experienced before. They are different. They’re driven by inflammatory and hormonal biology, not by eating too much or not exercising enough.
I want to be clear about the framing here: this is not a weight loss discussion. The metabolic changes that accompany inflammation — insulin resistance, visceral fat accumulation, disrupted energy regulation — are the health concern, regardless of what the scale says. Addressing these through anti-inflammatory nutrition, movement, sleep, and stress management supports metabolic health in ways that caloric restriction alone simply doesn’t.
Fatigue
The exhaustion of perimenopause isn’t laziness. It’s not a motivation problem. And it’s not solved by caffeine.
Inflammatory chemicals trigger an evolutionary response called “sickness behavior” — your body redirecting energy toward immune function and healing. It includes fatigue, reduced motivation, and withdrawal. When you have an acute illness, this response helps you recover. But when inflammation is chronically elevated — as it is during perimenopause — this fatigue response becomes chronic too.
Layer in disrupted sleep, mood instability, and metabolic turbulence, and you get an exhaustion that no amount of coffee can touch. Because coffee doesn’t address the inflammatory drive underneath it.
The Insight That Changes Everything
Here it is: because all seven of these symptoms share a common inflammatory root, they respond to the same foundational approach. You don’t need seven separate strategies. You need one comprehensive anti-inflammatory framework, applied consistently.
This is genuinely empowering. Once you understand the connection, you stop chasing individual symptoms and start addressing the underlying mechanism. One dietary pattern. One lifestyle approach. Multiple symptoms improving in parallel.
The Four Anti-Inflammatory Pillars
Pillar 1: Anti-Inflammatory Nutrition
The dietary pattern that the research supports is plant-rich, anti-inflammatory, and includes regular whole soy foods, omega-3 fats, diverse fiber, fermented foods, and anti-inflammatory spices — while naturally reducing ultra-processed foods, added sugar, and excess alcohol.
This is essentially a Mediterranean-style eating pattern. It’s the pattern used in the WAVS trial. It’s what the Dietary Inflammatory Index research points toward. And a 2024 study found that Australian women with the highest adherence to this pattern had 80% lower odds of moderate-to-severe hot flashes (Byrne-Kirk et al., 2024).
The principle is nutrition by addition — not restriction. You’re not “going on a diet.” You’re adding more of what calms inflammation and naturally displacing what fuels it.
| Add More Of | Why It Matters |
|---|---|
| Whole soy (edamame, tofu, tempeh, miso) | Isoflavones with anti-inflammatory and phytoestrogenic properties |
| Ground flaxseed (2 tbsp daily) | Lignans, omega-3s, and fiber in one food |
| Fatty fish — SMASH fish (salmon, mackerel, anchovies, sardines, herring) | EPA and DHA reduce inflammatory markers directly |
| Extra virgin |
Oleocanthal has ibuprofen-like anti-inflammatory activity |
| Deeply colored fruits and vegetables | Polyphenols, anthocyanins, and carotenoids that interrupt inflammatory pathways |
| Fermented foods (yogurt, kefir, kimchi, sauerkraut, miso) | Support the gut bacteria that may determine how well soy works for your symptoms |
| Turmeric with black pepper | Curcumin is one of the most studied anti-inflammatory compounds; piperine enhances absorption |
For a full week of meals built around these principles, see my 7-day anti-inflammatory meal plan for perimenopause.
Pillar 2: Consistent Movement
This doesn’t mean training for a marathon. Regular moderate activity — walking, swimming, cycling, yoga — has anti-inflammatory effects that are independent of weight changes. Resistance training is particularly important during perimenopause for preserving muscle mass and bone density, both of which decline with falling estrogen.
The key word is consistent. Thirty minutes of daily walking measurably reduces inflammatory markers over time. Consistency beats intensity, every time.
Pillar 3: Sleep Optimization
Sleep is when your body performs its anti-inflammatory repair work. Prioritizing sleep during perimenopause isn’t a luxury — it’s a physiological requirement.
Practical strategies: keep your bedroom at 65-68°F, use moisture-wicking fabrics, reduce blue light exposure in the evening, consider magnesium glycinate as an evidence-supported sleep aid, and address underlying sleep disorders if present.
Pillar 4: Stress Management
Chronic stress elevates cortisol. Cortisol promotes inflammation. During perimenopause, when your primary anti-inflammatory buffer (estrogen) is declining, the inflammatory impact of stress is amplified.
This doesn’t mean you need to eliminate stress from your life. It means consistent practices — deep breathing, time in nature, gentle movement, creative expression, structured mindfulness, or whatever works for you — that give your nervous system regular opportunities to downshift.
The Positive Cycle
These four pillars work synergistically. Better nutrition supports better sleep. Better sleep reduces cortisol. Lower cortisol reduces inflammation. Less inflammation means fewer symptoms across all seven categories. It’s a positive cycle — the exact reverse of the vicious one you may be caught in right now.
Where to Start (Without Getting Overwhelmed)
If all of this feels like a lot, I hear you. Here’s the simplest possible path forward:
This week: Pick one pillar. Just one. If you’re not sure which, start with food — you make choices about it multiple times a day. Add two tablespoons of ground flaxseed to your morning meal. Add one fermented food to your daily routine. Use extra virgin
Next week: Add a second pillar. If sleep is suffering, address your bedroom temperature and try magnesium glycinate at bedtime. If movement has dropped off, commit to a 20-minute daily walk.
Week three and beyond: Build gradually. Track your symptoms. Notice what changes first. For most women, sleep and energy tend to improve before other symptoms — and those improvements create momentum for everything else.
And if you want the simplest possible entry point, my 5 anti-inflammatory swaps for women over 40 takes less than five minutes to read.
When to See Your Doctor
An anti-inflammatory lifestyle approach is a complement to medical care — not a replacement. Please consult your healthcare provider if:
- Your symptoms are significantly affecting your quality of life or daily functioning
- You’re experiencing new joint pain that could indicate a specific inflammatory condition
- Cognitive changes are persistent, progressive, or accompanied by other neurological symptoms
- Mood changes include thoughts of self-harm or significant depression
- Sleep disruption is severe, or involves snoring, gasping, or excessive daytime sleepiness
- You’re interested in hormone therapy or other medical interventions
These conversations matter, and anti-inflammatory nutrition works alongside whatever your provider recommends. (Not sure how to bring up nutrition with your doctor? I wrote a guide on how to talk to your doctor about anti-inflammatory nutrition for menopause, including conversation scripts and a research summary you can bring to your appointment.)
You Are Not Falling Apart
I want to leave you with this.
You are not falling apart. You are not “just getting old.” Your body is going through a measurable, documented inflammatory shift — one that the medical system typically addresses piecemeal, symptom by symptom, rather than as the connected whole it actually is.
The fact that you’re reading this — that you’re learning what perimenopause actually does to your inflammatory pathways — puts you ahead of the vast majority of advice out there. Most women are never told this. You now know.
And knowing changes everything. Because instead of chasing seven separate problems, you can address one root mechanism. One dietary pattern. One lifestyle framework. Multiple symptoms improving together.
You deserve to know this. You deserve to feel supported during a transition that affects far more than what you’ve been told. And you absolutely have the power to influence how your body moves through it.
So — what’s the one thing you’ll try this week?
This article is for educational purposes and is not a substitute for personalized medical advice. If your symptoms are significantly affecting your quality of life, please consult with your healthcare provider about the full range of options available to you, including hormone therapy. An anti-inflammatory approach can complement — not replace — appropriate medical care. (Not sure how to start that conversation? See my guide on how to talk to your doctor about anti-inflammatory nutrition for menopause.)
References (click to expand)
Barnard, N. D., Kahleova, H., Holtz, D. N., Znayenko-Miller, T., Sutton, M., Holubkov, R., … & Setchell, K. D. R. (2023). A dietary intervention for vasomotor symptoms of menopause: A randomized, controlled trial. *Menopause*, 30(1), 80-87. [https://doi.org/10.1097/GME.0000000000002080](https://doi.org/10.1097/GME.0000000000002080)
Byrne-Kirk, G., Mantzioris, E., Scannell, N., & Villani, A. (2024). Adherence to a Mediterranean-style diet and severity of menopausal symptoms in perimenopausal and menopausal women from Australia: A cross-sectional analysis. *European Journal of Nutrition*, 63(7), 2743-2751. [https://doi.org/10.1007/s00394-024-03462-3](https://doi.org/10.1007/s00394-024-03462-3)
El Khoudary, S. R., Chen, X., Qi, M., Matthews, K. A., Karlamangla, A. S., Gold, E. B., … & Greendale, G. A. (2025). The relation between systemic inflammation and the menopause transition: The Study of Women’s Health Across the Nation. *Journal of Clinical Endocrinology & Metabolism*, 110(11), e3566-e3576. [https://doi.org/10.1210/clinem/dgaf175](https://doi.org/10.1210/clinem/dgaf175)
El Khoudary, S. R., Greendale, G., Crawford, S. L., et al. (2019). The menopause transition and women’s health at midlife: A progress report from the Study of Women’s Health Across the Nation (SWAN). *Menopause*, 26(10), 1213-1227. [https://doi.org/10.1097/GME.0000000000001424](https://doi.org/10.1097/GME.0000000000001424)
Haghshenas, N., Baharanchi, F. H., Melekoglu, E., Sohouli, M. H., & Shidfar, F. (2023). Comparison of predictive effect of the dietary inflammatory index and empirically derived food-based dietary inflammatory index on the menopause-specific quality of life and its complications. *BMC Women’s Health*, 23(1), 349. [https://doi.org/10.1186/s12905-023-02485-y](https://doi.org/10.1186/s12905-023-02485-y)
McCarthy, M., & Raval, A. P. (2020). The peri-menopause in a woman’s life: A systemic inflammatory phase that enables later neurodegenerative disease. *Journal of Neuroinflammation*, 17, 317. [https://doi.org/10.1186/s12974-020-01998-9](https://doi.org/10.1186/s12974-020-01998-9)
Monteleone, P., Mascagni, G., Giannini, A., Genazzani, A. R., & Simoncini, T. (2018). Symptoms of menopause — global prevalence, physiology and implications. *Nature Reviews Endocrinology*, 14(4), 199-215. [https://doi.org/10.1038/nrendo.2017.180](https://doi.org/10.1038/nrendo.2017.180)
Santoro, N., Epperson, C. N., & Mathews, S. B. (2015). Menopausal symptoms and their management. *Endocrinology and Metabolism Clinics of North America*, 44(3), 497-515. [https://doi.org/10.1016/j.ecl.2015.05.001](https://doi.org/10.1016/j.ecl.2015.05.001)
Zhang, Z., et al. (2024). Estrogen-immuno-neuromodulation disorders in menopausal depression. *Journal of Neuroinflammation*, 21, 159. [https://doi.org/10.1186/s12974-024-03152-1](https://doi.org/10.1186/s12974-024-03152-1)